Vitreous Hemorrhage
What is a vitreous hemorrhage?
The vitreous gel occupies approximately 2/3 of the total volume of the eye. Furthermore, it is a semisolid or liquid clear substance that fills the space between the lens in the front of the eye and the retina lining the back of the eye. Additionally, there are normally no blood vessels within the vitreous gel. Abnormal blood vessels can grow into the vitreous gel in a variety of eye diseases, most commonly diabetic retinopathy. There are, of course, many blood vessels surrounding the vitreous gel. A vitreous hemorrhage occurs when a blood vessel ruptures and bleeds within or near the vitreous cavity
Vitreous Hemorrhage Symptoms
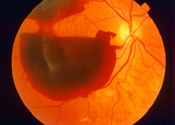
What happens if a vitreous hemorrhage is left untreated?
A vitreous hemorrhage may result from proliferative retinopathy, the condition in which new, abnormal blood vessels grow on the surface of the retina. This is referred to as neovascularization. When not treated, these new blood vessels may continue to grow and spread through the vitreous onto the pupil area. This can increase ocular pressure (pressure within the eye) that presses on the optic nerve. Damage to the optic nerve is irreparable and can lead to vision loss. Bleeding from a vitreous hemorrhage can also cause scar tissue to form near the back of the eye. This can pull the retina away from the back lining of the eye, requiring additional treatment to keep the retina from detaching and permanently damaging vision.
Is a vitreous hemorrhage painful?
No. This is one of the reasons why ophthalmologists are greatly concerned about increasing awareness about this condition. In many cases, a vitreous hemorrhage can develop very quickly and without pain that indicates a medical emergency.
An ophthalmologist or nearby emergency room should be contacted promptly if symptoms of vitreous hemorrhages, such as sudden floaters or cobwebs in vision or a red or shadowy effect, occur.
How long does it take for vitreous hemorrhage to clear?
How long it takes for symptoms of a vitreous hemorrhage to clear depends on the cause and severity of the bleed. Once the source of bleeding is found, treatment can be conducted. Small vitreous hemorrhages may be treatable with a laser treatment that repairs the bleeding vessels and tears in the retina, if applicable. Once the source of bleeding has been repaired, it can take several weeks for the blood that has accumulated in the eye to clear.
Diagnosing Vitreous Hemorrhage At Vitreo Retinal Surgery
Our doctors at Retina Consultants of Minnesota in Minneapolis, MN will examine the patient’s eyes as well as review their medical history to determine the cause of the hemorrhage. We will recommend the appropriate treatment. To confirm the diagnosis, a series of diagnostic tests may be performed such as:
- B-scan
- Gonioscopy
- Dilated eye examination
- IOP
- Indirect ophthalmoscopy
- Slit-lamp examination
What Causes Vitreous Hemorrhage?
There are many possible causes of vitreous hemorrhage, including systemic diseases such as:
- Diabetes mellitus
- Sickle cell anemia
Also, with aging the vitreous gel liquefies and separates from the retina, creating a posterior vitreous detachment. Bleeding can sometimes be associated when this occurs. Other causes of vitreous hemorrhage include ocular trauma, retinal tears or detachment, retinal vein occlusion, other vascular abnormalities, tumors, and rarely wet macular degeneration.
Our Treatment Options For Vitreous Hemorrhage
The most important issue is the prompt evaluation of an eye with an acute vitreous hemorrhage to determine the cause and to determine the status and health of the retina. Our team uses diagnostic ultrasonography equipment to study the inside of your eye in situations where there is too much blood to allow for direct visualization of the retina. Depending on the situation, we may initially observe a vitreous hemorrhage to see if the body will absorb it on its own. Sometimes we may require vitrectomy surgery to remove the blood, improve vision, and to address any underlying retinal disease.
Patient Testimonials
“October 2013 Surgery went very well. I was pleased with the amount of detail I was provided about the eye condition and treatment options, and with the pre-surgery instructions and the surgery. It healed quickly and successfully, with no complications. I had prepared questions and she answered them thoroughly.”
Why is the vitrectomy surgery procedure used to remove blood from the vitreous hemorrhage?
A vitrectomy is an eye procedure that corrects problems in the vitreous and retina. It works by removing the unhealthy vitreous and replacing it with a suitable substance. The vitreous is a gel-like matter that fills the center area of the eye. During the surgery, the ophthalmologist severs the vitreous from the retina and carefully suctions the gelatinous matter out of the eye. If other repairs are needed, such as a retinal tear, correction is made before gas or air is inserted to take the place of the vitreous.
Is there any recovery from the vitrectomy surgery for a vitreous hemorrhage?
Ophthalmologists provide clear post-operative instructions to each patient based on their case. Most vitrectomies are performed on an outpatient basis. Patients will need someone to drive them home after their procedure. To facilitate optimal healing, patients may need to use antibiotic eye drops daily for a short time after their vitrectomy. An eye patch may also be worn for a few days. The eye may be slightly sore, but this is typically manageable with over-the-counter pain medication. If a gas bubble replaces the vitreous, it is necessary to follow specific instructions provided by the surgeon.
After a vitrectomy, patients will need to avoid air travel for some time. A follow-up is scheduled for the day after the procedure or shortly thereafter to evaluate healing and surgical success. At that time, the doctor may have information about when it is safe to fly and resume other activities that may affect eye pressure.
Schedule a Consultation
To learn more about diabetic retinopathy, please call (855) 515-2020 to schedule a consultation.
We are proud to serve the communities of Minneapolis/St Paul, Brainerd, Duluth, Glencoe, Mankato, St. Cloud, and more.


