Retinal Tears & Detachments
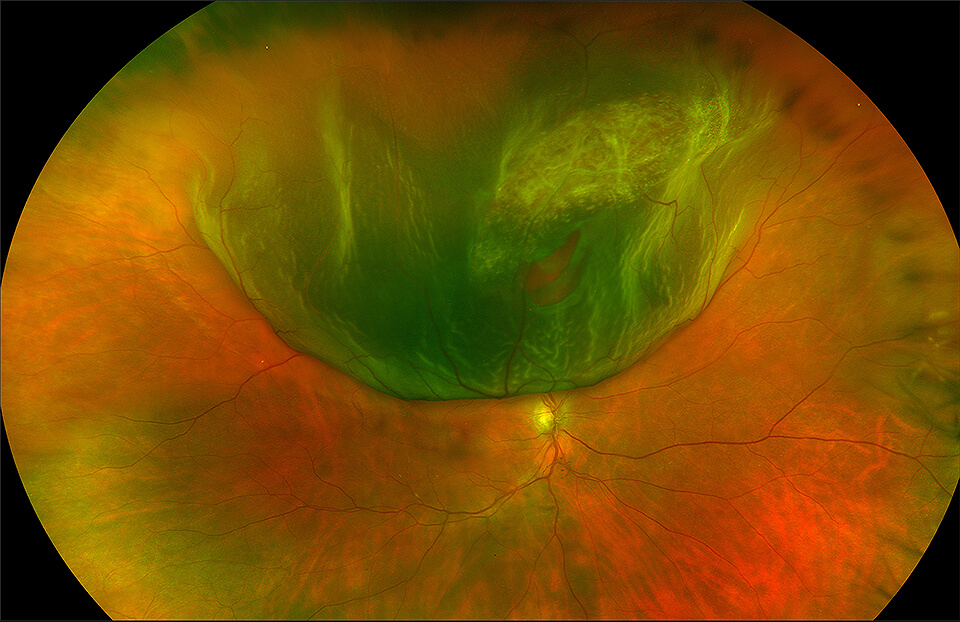
A retinal tear usually occurs as a spontaneous development in an eye as a result of a posterior vitreous separation (PVS) unrelated to anything the person has done.
What is A Retina?
The retina is the nerve layer that lines the back of the eye. If you think of the eye as a camera, the retina is the film in the camera. A clear gel called the vitreous, located just in front of the retina fills up the inside cavity of the eye. As one age, the vitreous gel contracts and liquefies. As this occurs, the vitreous gel may sometimes pull a tear in the retina. Fluid from inside the eye can leak through the tear, and the retina can separate from the back wall of the eye, creating a retinal detachment.
What is A Retinal Tear?
The eye is a very complex functional and anatomic organ. The retina is a thin, delicate and transparent sheet of tissue that lines the inside of the back of the eye. Directly in front of the retina is a cavity that contains a gel called vitreous, a complex structure consisting of aqueous fluid, macromolecules and collagen fibrils. In children, the vitreous is an optically clear, transparent and formed gel. However, as life progresses, the vitreous gel naturally and gradually liquifies. By mid to late life, the vitreous has mostly liquified except for a layer of gel up against the retina. At some point in nearly all people, this layer of gel will spontaneously begin to peel away or separate from the retina. This natural development in the eye is called a posterior vitreous separation (PVS). In most cases, the vitreous gel peels cleanly away from the retina and the PVS occurs without vision threatening consequences. However, in some eyes, the vitreous gel may be more adherent to some areas of the retina than others and when it peels away from these more adherent areas, it may pull hard enough to cause a retinal tear. Once a retinal tear has developed, vitreous fluid can go through the tear leading to a retinal detachment.
Many people experience no symptoms from a PVS or retinal tear, and a PVS does not always lead to a retinal tear. However, when symptoms do occur, they most commonly consist of flashing lights and/or the sudden onset of floaters in the vision of the affected eye. These symptoms should always prompt a careful and complete examination of the back of the eye and the retina within a day or two of onset. If a retinal tear is identified before a retinal detachment has begun to occur, laser can be used to seal the edges of the tear and decrease the risk of retinal detachment. However, if a retinal detachment has already begun, the eye will usually require surgery to prevent blindness.
People often ask what they did to cause a retinal tear to develop or if a bump to the head or minor eye trauma caused the retinal tear. The fact is that the vast majority of retinal tears occur spontaneously due to the above noted anatomical developments. Falls, bumps to the head and minor eye trauma do not usually cause retinal tears. However, a severe blow directly to the eye can sometimes cause a retinal tear and such severe direct blows should prompt a careful examination of the retina by a specialist.
The Symptoms of Retinal Detachment
Retinal detachment may progress slowly or rapidly, but both should be reported to a medical doctor as soon as possible so as to minimize the risk of vision loss. As there is no pain with retinal detachment, some of the symptoms include the following:
- A sudden decrease in visual acuity
- A sudden increase in the amount of “floaters” in vision
- Bright flashes in the periphery
- An unnatural “curving” of straight lines
- Loss of central vision
- A dense shadow throughout the visual field
What Causes Retinal Detachment?
Retinal detachments occur with a frequency of 1 per 10,000 people per year. It is a serious condition that may lead to blindness if not treated appropriately. Retinal detachment can be a complication of cataract surgery. Severe inflammation may alter the position of the retinal tissue and begin the detachment process. Other risk factors include the following:
- Nearsightedness (myopia)
- A retinal tear
- Family history of retinal detachment
- Glaucoma
- Cataract surgery
- Trauma
- Existing eye condition
- Retinal detachment in the other eye
Weak areas in the retina such as lattice degeneration can also be a risk factor of retinal detachment.
Early Signs of Retinal Detachment:
Floaters
Floaters are a typical part of aging, but they can also signal a possible case of retinal detachment. As their name implies, floaters appear to float around in front of your field of vision. They look like wavy lines, dots, circles, small specks, or even cobwebs. It appears they are at the front of the eye and you are seeing through them, but what you are seeing is actually the shadow cast on the retina by the floaters.
Floaters are tiny clumps of gel or cells inside the vitreous, a clear gel-like substance that fills the eye. Because the retina, which interprets the images that enter the eye through the cornea, is at the back of the eye, the light comes into the eye and floaters cast shadows onto the retina. They are most evident when you’re looking at a plain background such as a clear blue sky, a white wall, or a blank computer screen. Floaters aren’t usually seen in darker light conditions.
What Causes Someone To Get Floaters?
Floaters form with aging, as the vitreous starts to liquefy and possibly shrink. This can lead to the formation of clumps and strands — floaters — and it can make the vitreous pull away from the back of the eye. Professionals refer to this as posterior vitreous detachment, and it usually leads to the development of floaters. This vitreous detachment is not usually serious.
However, if the vitreous detachment pulls on the retina, it can create a tear in the retina and can lead to retinal detachment. This can create new floaters, especially small spots. A sudden increase in floaters can be a sign of retinal detachment.
How is Retinal Detachment diagnosed?
Diagnosis of a retinal detachment is made after a thorough medical eye examination and the performance of the following diagnostic tests:
- Dilated eye examination
- Ultrasound of the eye
- Fundus photography of the retina
- Visual acuity test
- Slit-lamp examination
- Electroretinogram
- Fluorescein angiography
- Ophthalmoscopy
Retinal Detachment Treatment
Retinal detachment repair brings the retina back into position and then sealing the hole or tear in the retina. Retinal detachment is almost always treated with some form of surgery. If the detachment is not extensive, laser treatment or cryotherapy (freezing) in the office are options. A procedure called pneumatic retinopexy treats some detachments. This involves the injection of air or gas into the eye in conjunction with laser or cryo. Doctors provide patients with specific head position instructions which allow the bubble to float up against the retina and keep it in position as it heals. Pneumatic retinopexy is only suitable for a select group of retinal detachments.
One of the most common surgical techniques in retinal detachment repair is a scleral buckle procedure. This is an operating room procedure in which a silicone band is placed around the eye. The band changes the shape of the eye and brings the retina back into contact with the wall of the eye. Then, cryo or lasers treat the retinal breaks and other weak areas.
Vitrectomy surgery also has a role in retinal detachment repair. This technique removes the vitreous gel and any scar tissue from the eye. After the retina reattachment, a gas bubble fills the vitreous cavity to help hold the retina in position. The bubble generally lasts in the eye for several weeks and is gradually absorbed by the body. A silicone oil bubble is an alternative to an oil bubble in more complex cases. Once the retinal tissues are stable, a second surgery removes the silicone oil because it does not dissolve on its own.
Retinal Detachment Surgery
Surgery for most retinal detachments takes about one hour and local anesthesia is an option. Although hospital admission is not necessary, your surgeon may give you specific instructions regarding head positioning in order to maximize the chances of a successful outcome. Surgeries involving gas bubbles usually include limitations on flying in an airplane or traveling to high altitudes. Also, if you need surgery for any other reason while a gas bubble is in the eye, it is important to notify the anesthesiologist to prevent the gas bubble from expanding in the eye.
What kind of results can I Expect?
The visual results of retinal reattachment depend on three main factors: how long the retina has been detached, how much of the retina has been detached, and most importantly, whether the center of vision has been involved. If the surgery does not involve the center of vision, nearly full visual recovery is more likely. If the surgery does involve the center of vision, there is usually some permanent loss of vision. Your prescription for glasses may also need adjustments as a result of the surgery.
Schedule a Consultation
To learn more about diabetic retinopathy, please call (855) 515-2020 to schedule a consultation.
We are proud to serve the communities of Minneapolis/St Paul, Brainerd, Duluth, Glencoe, Mankato, St. Cloud, and more.


