Epiretinal Membrane
What is an epiretinal membrane?
An epiretinal membrane is a thin sheet of fibrous tissue that can develop on the surface of the macular area of the retina and cause a disturbance in vision. An epiretinal membrane is also sometimes called a macular pucker, macular fibrosis, surface wrinkling retinopathy or cellophane maculopathy. The retina is a clear film of very delicate tissue that lines the inside of the back of the eye. The macula is in the center of the retina and it gives us sharp central vision and reading vision.
What causes an epiretinal membrane?
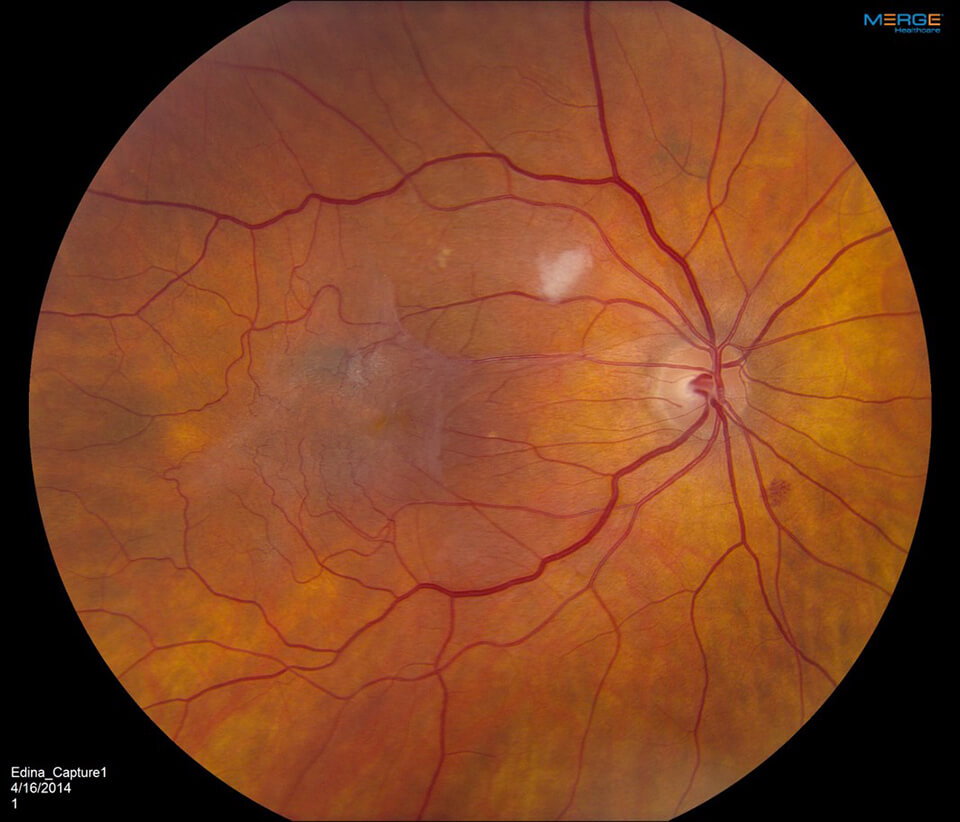
An epiretinal membrane develops as a result of cellular changes that occur in the back of the eye between the clear vitreous gel that is normally present, and the macula. Normal biological cells derived from the retina and other tissues within the eye become liberated into the vitreous gel and eventually settle onto the surface of the macula. These cells may begin to proliferate into a “membrane.” In many instances, this membrane remains very mild and does not have any significant effect on the macula or the person’s vision. In other cases, however, the membrane may slowly become more prominent, eventually creating a disturbance in the retina that leads to visual blurring and/or distortion in the affected eye.
In the majority of cases, an epiretinal membrane develops in an eye with no history of previous problems. This type of epiretinal membrane is called idiopathic. Occasionally, however, an epiretinal membrane will develop in an eye as a result of retinal detachment, trauma, inflammatory disease, blood vessel abnormalities, or other pathological conditions. Most epiretinal membranes are mild and have little or no effect on vision. However, in some cases, the epiretinal membrane may slowly grow and begin to cause mechanical distortion (“wrinkling”) in the macula. This may lead to blurred or distorted vision, which may slowly worsen over time. An epiretinal membrane does not make an eye go completely blind. It typically affects only the center area of vision and does not cause a loss of the peripheral (side) vision.
Epiretinal Membrane Treatment
Epiretinal membranes can be treated with vitrectomy surgery. However, not all epiretinal membranes require treatment. Surgery is not necessary if the epiretinal membrane is mild and having little or no effect on vision. There is no non-surgical treatment for an epiretinal membrane.
Vitrectomy Surgery
Vitrectomy surgery is usually done on an outpatient basis under local anesthesia. The surgery consists of making very small incisions on the white part of the eye (the sclera) 4 mm behind the edge of the cornea. While looking into the eye through a microscope, the surgeon can use a variety of specialized instruments to work within the eye. First, the vitreous gel is removed and replaced with a specially designed saline solution. The surgeon can then “peel” the membrane from the surface of the macula. After surgery, very fine absorbable sutures close the incisions.
Newer surgical techniques and instrumentation may allow the surgeon to perform the surgery in some cases through tiny “self-sealing” incisions that do not require sutures. This new technique allows for faster healing of the eye with minimal post-operative ocular irritation. A patch goes over the eye following surgery and stays in place until the next day.
Vitrectomy Surgery Recovery
Eye drops or ointment are necessary for several weeks after surgery to facilitate healing. Following surgery, patients can usually resume normal non-strenuous physical activities the next day. How quickly the patient can drive, return to work, perform fine visual tasks, or engage in strenuous activities varies from person to person.
Results Of Epiretinal Membrane Surgery
Most patients will have a significant improvement in vision after surgery, however, this may occur gradually over several months. The amount of visual improvement varies from person to person and depends on multiple factors including the severity and chronicity of the epiretinal membrane, the level of vision preoperatively, and the presence of any other ocular abnormalities.
Risks And Complications With Vitrectomy Surgery
Any surgical procedure carries a risk of complications and epiretinal membrane surgery is no exception. Post-operative infection (endophthalmitis) can be very serious and may lead to blindness in the affected eye. Most infections can be effectively treated if identified at an early stage. Endophthalmitis is rare and occurs in approximately 1 out of 1000 cases. In addition, retinal detachment is another complication that can cause blindness if not treated. Retinal detachments occur in 1 to 2 out of 100 cases following epiretinal membrane surgery.
Finally, the progression of cataract is a third consideration. A cataract occurs when the lens in the eye becomes cloudy. This typically occurs with aging but is accelerated by vitrectomy surgery. This is not a concern if the patient has already had cataract surgery prior to vitrectomy surgery. Other risks of surgery include bleeding, loss of vision, double vision, scarring, a droopy eyelid, and anesthetic complications. Your surgeon will review the risks and benefits of surgery with you.
Schedule a Consultation
To learn more about diabetic retinopathy, please call (855) 515-2020 to schedule a consultation.
We are proud to serve the communities of Minneapolis/St Paul, Brainerd, Duluth, Glencoe, Mankato, St. Cloud, and more.


